Masks During the COVID-19 Pandemic
Masking Efficacy Research
Prior Research on Preventing Viral Transmission Using Masks
COVID-19 Specific Masking Research
Negative
https://www.maskscience.org/
https://www.legis.nd.gov/assembly/67-2021/testimony/HPOLSUB-1323-20210204-5273-F-SEELY_BRADLEY.pdf
https://www.medrxiv.org/content/10.1101/2023.07.07.23292338v1.full
Positive
Other
A discussion in the BMJ, from November 2020, of the weird responses to the infamous DANMASK-19 Danish mask study.
This is an Unherd interview with Carl Heneghan, (Professor of Evidence-Based Medicine, University of Oxford, Editor In Chief with BMJ Evidence-Based Medicine) and Tom Jefferson, epidemiologist from the Cochrane Centre and Honorary Senior Research Fellow, Centre For Evidence Based Medicine, University of Oxford.
Here are a couple of pertinent quotes;
“Specifically on masks, there is no evidence, aside from people who are exposed on the frontlines, that masks make any difference, but that is extraordinary on its own, but what is even more extraordinary is that what I’m describing is uncertainty: we don’t know if these things make any difference.”
Asked about studies that show how much masks can reduce the spread of particles…
“We’re dealing with some of the most slippery customers in the market – respiratory viruses. It’s not just a question of the bug and the person, it’s also the setting which is why all these laboratory based experiments … looking at the plume of droplets coming out of Mask A versus Mask B and so on have to be treated with extreme care. What we really should be doing is experiments – trials – in the population, and we have to do them when there is virus circulating.” (He says earlier that it can’t be done now because virus circulation is low).
Asked about isn’t this common sense – do you believe a face covering reduces the amount of virus that can be transmitted?
“The problem with that particular belief is that the one arm of a randomised controlled trial that was published in 2015 – so one section of the people who took part in this study in south-east Asia – wore cloth masks, and they found that these cloth masks not only didn’t work, but actually, probably, saliva, the secretions and the wetness made them more permeable to incoming agents.”
Meta-Analysis and Research Aggregation
- Paul Alexander's list of 150 comparative studies and articles on mask (in)efficacy and harm.1)
Societal Impacts of Masking
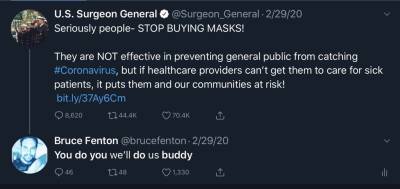
It's important to remember how, in the early days of the pandemic, we were specifically told not to wear masks, as they are not effective against Covid-19. Here's a tweet from the US Surgeon General that was later deleted;
And here is Dr. Hilary, on UK television, explaining why masks don't protect anyone and, furthermore, can actually cause health issues and problems. (He did a more forceful version of this on the same programme, at a later date, but it appears to have been removed. It can be seen, however, towards the bottom of this article on a TV poll on vaccine mandates that went 89% to the No's before being taken down). He very quickly took the opposite position, presumably once the “error of his ways” was pointed out to him.
The pro-mask response to these early messages is that the world was short of PPE equipment at the time, and therefore what little we had available needed to be reserved for medical frontline workers. While that makes a certain amount of sense (leaving aside the fact that much of the 'preparedness' measures that arose from the many pandemic war games that were run over many years, like Event 201, appear to have been ignored), these messages do demonstrate the willingness of our health authorities and certain doctors to lie to us to serve a particular agenda.
Which leaves us wondering - were they lying then? Or are they lying now?
Here we break down all relevant medical literature and testimony to determine not only the effectiveness of cloth, N95, and surgical masks, but to describe the negative psychological impacts to children and society as a whole.
Prior to SARS-CoV-2, there have been a number of studies on various masks and they're ability to reduce the spread of common respiratory viruses:
https://www.rcreader.com/commentary/masks-dont-work-covid-a-review-of-science-relevant-to-covide-19-social-policy
https://www.youtube.com/watch?v=z_uMYfemmJM
Debunking of Debunking of Rancourt: https://www.researchgate.net/publication/343263629_A_Complete_Debunking_of_Denis_Rancourt's_Mask_Don't_Work
Lancet 2022 Mask Study
Revisiting Pediatric COVID-19 Cases in Counties With and Without School Mask Requirements—United States, July 1—October 20 2021 - 11 Pages Posted: 25 May 2022 - Ambarish Chandra - University of Toronto Tracy Beth Høeg - University of California, Davis; MD, PhD
Findings: Replicating the CDC study shows similar results; however, incorporating a larger sample and longer period showed no significant relationship between mask mandates and case rates. These results persisted when using regression methods to control for differences across districts. Interpretation: School districts that choose to mandate masks are likely to be systematically different from those that do not in multiple, often unobserved, ways. We failed to establish a relationship between school masking and pediatric cases using the same methods but a larger, more nationally diverse population over a longer interval. Our study demonstrates that observational studies of interventions with small to moderate effect sizes are prone to bias caused by selection and omitted variables. Randomized studies can more reliably inform public health policy.
Funding: University of Toronto 2)
An Industrial Hygienist's View
Industrial Hygiene (IH) is the field concerned with exposures, personal protective equipment (PPE) and warnings about exposures, as well as their management in all sorts of settings, not just workplace but also schools and other places.
Stephen E Petty is an industrial hygienist with extensive experience who has testified on many occasions on the topic of public safety and protection; here is an example on masks in the pandemic:
https://notcbc.ca/2022/05/14/expert-on-masks-and-ppe-masks-dont-stop-or-slow-viral-spread/
Essentially, he explains that virions such as SARS-COV-2 are much too small to be stopped by cloth or surgical masks. These masks have gaps around them such that the aerosols transmitting viruses will not be stopped at all. N95s may reduce risk of contracting SARS-COV-2 but must be used under the Respiratory Protection Standard as defined by OSHO 29 CFR 1910.134, elements of which include fitting annually, and training on proper use and storage (see also the above presentation jan 27, 2022).
Petty also describes IH or “engineering controls” that can address exposure control – “Dilution by ventilation or maximum fresh air”.